 Bioidentical Hormones Found Beneficial After Hysterectomy
Bioidentical Hormones Found Beneficial After Hysterectomyby Jeffrey Dach MD
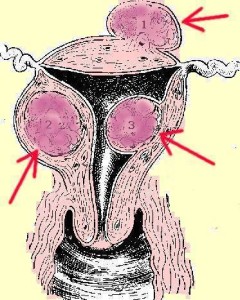
Shirley was a Forty Three year old executive for an internet company. She came to see me because of irregular bleeding from massive uterine fibroids. (see image at left).
The continuous bleeding interfered with her lifestyle and caused severe fatigue from the iron deficiency anemia. I had proposed a procedure called hysterectomy because the fibroids were very large. Shirley went home, and after thinking for a few days, finally accepted she would go see her OB/Gyne surgeon to schedule the operation.
Left image: Diagram of cross section of uterus. Red Arrows point to uterine fibroids . Courtesy of wikimedia commons.
Uterine fibroids are benign growths in the uterus that sometimes enlarge and cause irregular bleeding, and pressure symptoms. They are fairly common and can be detected with pelvic examination, and confirmed with pelvic sonogram and MRI scan. Massive uterine fibroids are most commonly treated with a surgical procedure called hysterectomy which removes the uterus and fibroid tumors. Treatment is usually successful with a good outcome.
Next, Shirley paid a visit to the OB GYNE surgeon to discuss her operation. The surgeon recommended a COMPLETE hysterectomy with removal of both ovaries. Sitting in the surgeon’s office, Shirley timidly protested. “Why remove my ovaries?” asked Shirley. The surgeon replied, “Removing the ovaries eliminates the chance of ovarian cancer, and you don’t need them anyway.”
So now Shirley was again in my office asking for my opinion. Should she go against the surgeon’s advice and insist on preserving her ovaries, or should she follow the surgeon’s advice to have a COMPLETE hysterectomy with removal of the ovaries ?
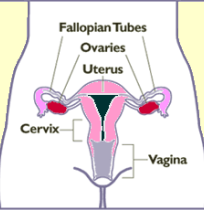 Left Image : Diagram showing Ovaries (in red). Uterus is Pink. Courtesy of Wikimedia Commons.
Left Image : Diagram showing Ovaries (in red). Uterus is Pink. Courtesy of Wikimedia Commons.
The ovaries are important because they are the hormone factories that pump out women’s hormones on a daily basis. Removing the ovaries removes the source of women’s hormones causing all hormone levels to decline to low levels, immediately sending the woman into Menopause.
Luckily, the answer to Shirley’s question can be found in the medical literature. William Parker MD and Cathleen Rivera MD reported that removing the ovaries is detrimental to overall health and results in increased mortality. (1)(2)
 Left image: Surgeons performing hysterectomy courtesy of wikimedia commons.
Left image: Surgeons performing hysterectomy courtesy of wikimedia commons.
Dr. Parker followed 30,000 women for 24 years after their hysterectomy. Half the patients had the ovaries removed and half had ovaries preserved. The group with ovaries removed did, in fact, have a lower rate of ovarian and breast cancer. However, this was overshadowed by a marked increase in death from heart disease and other cancers. The group with the ovaries removed had a higher all cause mortality rate, and therefore Dr. Parker recommended that women preserve the ovaries in the pre-Menopausal age group. Dr Parker also found that postoperative hormone replacement is very beneficial at reducing heart disease risk. (1)
In a second study, Dr Cathleen Rivera followed 1,000 Pre-Menopausal women (under age 45) after hysterectomy, and found that removal of the ovaries resulted in a disturbing 84% increase in death from heart disease. However, if these women were given estrogen replacement after ovarian removal, they were protected with a 35% decrease in mortality from heart disease.(2) I thought this was rather impressive.
These two studies provide convincing evidence of the health benefits of hormone replacement after hysterectomy. Although the patients in these two studies were given Premarin which is a natural hormone (from a pregnant horse), we find that a cocktail of bioidentical hormones including estradiol, estriol, progesterone, DHEA and testosterone works as well or better than the horse hormones. Since all women are humans, we I consider it preferable to prescribe human hormones rather than hormones from pregnant horse urine (Premarin).
 Left Image: pregnant horse, courtesy of wikimedia commons. Why use horse hormones when human hormones are available?
Left Image: pregnant horse, courtesy of wikimedia commons. Why use horse hormones when human hormones are available?
For women at high risk with familial breast and ovarian cancer, and positive BRCA genetic markers, Dr Parker says it makes sense to go ahead with removing the ovaries for these people in high risk groups.
Update 2013:
A new study published by Philip M. Sarrel, MD says that,(5)
“over a 10-year span, starting in 2002, a minimum of 18,601 and as many as 91,610 postmenopausal women died prematurely because of the avoidance of estrogen therapy (ET)…… Estrogen Therapy (ET) in younger postmenopausal women is associated with a decisive reduction in all-cause mortality, ” (5)
Articles with Related Interest:
The Safety of Bio-Identical Hormones
The Importance of Bioidentical Hormones
Bioidentical Hormones Prevent Arthritis
Bioidentical Hormone Estrogen Prevents Heart Disease
Morning Rounds With Steven Economou MD
Waking Up from the Synthetic Hormone Nightmare
HRT Does Not Cause Breast Cancer
Jeffrey Dach MD
http://www.jeffreydach.com/
http://www.drdach.com/
http://www.naturalmedicine101.com/
http://www.truemedmd.com/
Links and References
(1) http://www.ncbi.nlm.nih.gov/pubmed/19384117
http://www.hgos.org/resources/OBGYN_Article.pdf
http://www.doctorsinfoweb.com/pdf/NHS_green_J_William_Parker-p1027.pdf
http://www.hopeforfibroids.org/pdf/NHS_green_J_William_Parker-p1027.pdf
Obstet Gynecol. 2009 May;113(5):1027-37.
Ovarian conservation at the time of hysterectomy and long-term health outcomes in the nurses’ health study. Parker WH, Broder MS, Chang E, Feskanich D, Farquhar C, Liu Z, Shoupe D, Berek JS, Hankinson S, Manson JE. John Wayne Cancer Institute at Saint John’s Health Center, Santa Monica, California 90401, USA. Comment in:
OBJECTIVE: To report long-term health outcomes and mortality after oophorectomy or ovarian conservation.
METHODS: We conducted a prospective, observational study of 29,380 women participants of the Nurses’ Health Study who had a hysterectomy for benign disease; 16,345 (55.6%) had hysterectomy with bilateral oophorectomy, and 13,035 (44.4%) had hysterectomy with ovarian conservation. We evaluated incident events or death due to coronary heart disease (CHD), stroke, breast cancer, ovarian cancer, lung cancer, colorectal cancer, total cancers, hip fracture, pulmonary embolus, and death from all causes.
RESULTS: Over 24 years of follow-up, for women with hysterectomy and bilateral oophorectomy compared with ovarian conservation, the multivariable hazard ratios (HRs) were 1.12 (95% confidence interval [CI] 1.03-1.21) for total mortality, 1.17 (95% CI 1.02-1.35) for fatal plus nonfatal CHD, and 1.14 (95% CI 0.98-1.33) for stroke. Although the risks of breast (HR 0.75, 95% CI 0.68-0.84), ovarian (HR 0.04, 95% CI 0.01-0.09, number needed to treat=220), and total cancers (HR 0.90, 95% CI 0.84-0.96) decreased after oophorectomy, lung cancer incidence (HR=1.26, 95% CI 1.02-1.56, number needed to harm=190), and total cancer mortality (HR=1.17, 95% CI 1.04-1.32) increased.
For those never having used estrogen therapy, bilateral oophorectomy before age 50 years was associated with an increased risk of all-cause mortality, CHD, and stroke. With an approximate 35-year life span after surgery, one additional death would be expected for every nine oophorectomies performed.
CONCLUSION: Compared with ovarian conservation, bilateral oophorectomy at the time of hysterectomy for benign disease is associated with a decreased risk of breast and ovarian cancer but an increased risk of all-cause mortality, fatal and nonfatal coronary heart disease, and lung cancer. In no analysis or age group was oophorectomy associated with increased survival.
(2) http://www.ncbi.nlm.nih.gov/pmc/articles/PMC2755630/?tool=pubmed
Menopause. 2009 Jan–Feb; 16(1): 15–23.
Increased cardiovascular mortality following early bilateral oophorectomy
Cathleen M. Rivera, MD,1 Brandon R. Grossardt, MS,2 Deborah J. Rhodes, MD,1 Robert D. Brown, Jr., MD, MPH,3 Véronique L. Roger, MD, MPH,4,5 L. Joseph Melton, III, MD, MPH,5 and Walter A. Rocca, MD, MPH3,5
We conducted a cohort study with long-term follow-up of women in Olmsted County, MN, who underwent either unilateral or bilateral oophorectomy before the onset of menopause from 1950 through 1987. Each member of the oophorectomy cohort was matched by age to a referent woman from the same population who had not undergone any oophorectomy. We studied the mortality associated with cardiovascular disease in a total of 1,274 women with unilateral oophorectomy, 1,091 women with bilateral oophorectomy, and 2,383 referent women.
Results: Women who underwent bilateral oophorectomy before age 45 years experienced an increased mortality associated with cardiovascular disease compared with referent women (HR, 1.44; 95% CI, 1.01–2.05; P = 0.04).
Within this age stratum, the HR for mortality was significantly elevated in women who were not treated with estrogen through age 45 years or longer (HR, 1.84; 95% CI, 1.27–2.68; P = 0.001) but not in women treated (HR, 0.65; 95% CI, 0.30–1.41; P = 0.28; test of interaction, P = 0.01). Mortality was further increased after excluding deaths associated with cerebrovascular causes.
Conclusions: Bilateral oophorectomy performed before age 45 years is associated with increased cardiovascular mortality, especially with cardiac mortality. However, estrogen treatment may reduce this risk.
From a clinical perspective, our findings suggest that women who underwent bilateral oophorectomy at a young age are at increased risk of cardiovascular death, especially of cardiac death. This increased mortality may be attenuated by adequate estrogen treatment. Our findings provide new evidence to guide the individualized assessment of the risks and benefits of prophylactic bilateral oophorectomy in young women.1,4–6,8,14 This preventive practice currently involves approximately 4.5 million women older than 55 years living in the United States who have undergone bilateral oophorectomy before reaching natural menopause.28,34
In addition, our findings provide observational evidence for a long-term cardiovascular protective effect of estrogen either naturally produced by the ovaries or given as treatment to women who underwent bilateral oophorectomy at younger ages. These findings emphasize the importance of estrogen treatment after the surgery.6,9–14
We focused our analyses on age at estrogen deficiency rather than on the length of estrogen treatment after the surgery to study the combined effects of age at the surgery and length of treatment.
Several studies have shown increased cardiovascular mortality in women who experienced early menopause (before age 45 years) from either natural or medical causes,35–40 and a statistical model has linked prophylactic bilateral oophorectomy before age 65 years with an increase in overall mortality and coronary heart disease mortality.1,4,5
Similarly, in the Women’s Health Initiative Observational Study, hysterectomy plus oophorectomy performed over a broad age range was a significant predictor of cardiovascular disease during a short-term follow-up.28
Recent analyses from the Women’s Health Initiative Coronary Artery Calcium Study showed an increased risk of subclinical coronary artery disease in women who underwent both hysterectomy and bilateral oophorectomy and were not treated with estrogen compared to women who underwent hysterectomy alone. The increased risk was independent of traditional cardiovascular risk factors.12
Our results for estrogen treatment after bilateral oophorectomy are consistent both with findings from previous clinical studies40–44 and with findings from animal studies. Primates who underwent premenopausal oophorectomy and did not receive exogenous estrogen had significantly accelerated atherosclerosis compared with those that did not have oophorectomy
This study showed that women who underwent early bilateral oophorectomy are at increased risk of death involving cardiovascular disease, especially cardiac diseases. However, treatment with estrogen through age 45 years or longer may reduce this risk. These findings, in conjunction with the results of other studies,1,4,5,8 have important clinical implications and should prompt a reassessment of prophylactic bilateral oophorectomy in premenopausal women.6,14
3) http://health.usnews.com/health-news/news/articles/2013/07/18/avoidance-of-hormone-therapy-may-have-harmed-hysterectomy-patients-study
Avoidance of Hormone Therapy May Have Harmed Hysterectomy Patients: Study
For older women without a uterus, estrogen may save lives, researchers say
By Kathleen Doheny HealthDay Reporter
4) http://www.medicaldaily.com/articles/17562/20130718/misconception-estrogen-therapy-50000-deaths-cancer-pogesterone.htm
Misconception About Estrogen Therapy Caused 50,000 Deaths of Women Post-Hysterectomy. By looking at the data researchers found that the media hype and misunderstanding of estrogen therapy has resulted in the premature death of 50,000 women who have had hysterectomies within the last decade.
By Jonathan Weiss, Ph.D. | Jul 18, 2013
5) http://ajph.aphapublications.org/doi/abs/10.2105/AJPH.2013.301295
The Mortality Toll of Estrogen Avoidance: An Analysis of Excess Deaths Among Hysterectomized Women Aged 50 to 59 Years Philip M. Sarrel, MD, Valentine Y. Njike, MD, MPH, Valentina Vinante, MD, and David L. Katz, MD, MPH
Published online ahead of print July 18, 2013
Objectives. We examined the effect of estrogen avoidance on mortality rates among hysterectomized women aged 50 to 59 years.
Methods. We derived a formula to relate the excess mortality among hysterectomized women aged 50 to 59 years assigned to placebo in the Women’s Health Initiative randomized controlled trial to the entire population of comparable women in the United States, incorporating the decline in estrogen use observed between 2002 and 2011.
Results. Over a 10-year span, starting in 2002, a minimum of 18 601 and as many as 91 610 postmenopausal women died prematurely because of the avoidance of estrogen therapy (ET).
Conclusions. ET in younger postmenopausal women is associated with a decisive reduction in all-cause mortality, but estrogen use in this population is low and continuing to fall. Our data indicate an associated annual mortality toll in the thousands of women aged 50 to 59 years. Informed discussion between these women and their health care providers about the effects of ET is a matter of considerable urgency. (Am J Public Health. Published online ahead of print July 18, 2013: e1-e6. doi:10.2105/AJPH.2013.301295)
http://www.businesswire.com/portal/site/home/permalink/?ndmViewId=news_view&newsId=20090420005411&newsLang=en
April 20, 2009 New Study Finds Removing Ovaries During Hysterectomy Increases Risk of Death, Outweighs Benefits
SANTA MONICA, Calif.–(BUSINESS WIRE)–Results of a landmark study led by a doctor at John Wayne Cancer Institute at Saint John’s Health Center raises serious questions about the long-term survival benefits of removing a woman’s ovaries during routine hysterectomy. The study, appearing in the May 2009 issue of Obstetrics and Gynecology, compared women with benign (noncancerous) reproductive disease who were given a hysterectomy, with either bilateral oophorectomy (removing both ovaries) or ovarian conservation (leaving the ovaries intact).
http://www.news-medical.net/news/2009/04/20/48588.aspx
Removal of ovaries during hysterectomy increases risk of death, outweighs benefits
20. April 2009 23:32
Jeffrey Dach MD
7450 Griffin Road Suite 180/190
Davie, Florida 33314
954-792-4663
http://www.jeffreydach.com/
http://www.drdach.com/
http://www.naturalmedicine101.com/
http://www.truemedmd.com/
Disclaimer click here: http://www.drdach.com/wst_page20.html
The reader is advised to discuss the comments on these pages with his/her personal physicians and to only act upon the advice of his/her personal physician. Also note that concerning an answer which appears as an electronically posted question, I am NOT creating a physician — patient relationship. Although identities will remain confidential as much as possible, as I can not control the media, I can not take responsibility for any breaches of confidentiality that may occur.
Link to this article:http://wp.me/P3gFbV-yW
Copyright (c) 2010, 2013 Jeffrey Dach MD All Rights Reserved. This article may be reproduced on the internet without permission, provided there is a link to this page and proper credit is given.
FAIR USE NOTICE: This site contains copyrighted material the use of which has not always been specifically authorized by the copyright owner. We are making such material available in our efforts to advance understanding of issues of significance. We believe this constitutes a ‘fair use’ of any such copyrighted material as provided for in section 107 of the US Copyright Law. In accordance with Title 17 U.S.C. Section 107, the material on this site is distributed without profit to those who have expressed a prior interest in receiving the included information for research and educational purposes.
FDA Approval for Paxil for Hot Flashes A Cruel Joke ? - Jeffrey Dach MD July 20, 2013 at 5:43 AM
[…] Bioids Hysterectomy […]
Bioidentical Hormones Reduce Mortality After Hysterectomy - Jeffrey Dach MD July 26, 2013 at 7:39 AM
[…] Bioids Hysterectomy […]
- Next Level Nutrition September 3, 2013 at 12:04 PM
[…] Bioidentical Hormones Beneficial After Hysterectomy […]
Newsweek Attacks Oprah Winfrey and BioIdentical Hormones - Next Level Nutrition September 3, 2013 at 12:20 PM
[…] Bioidentical Hormones Beneficial After Hysterectomy […]
More Misinformation on Bioidentical Hormones - Jeffrey Dach MD March 27, 2014 at 7:09 AM
[…] Bioidentical Hormones Found Beneficial After Hysterectomy […]