Riboflavin for Hypertension in MTHFR
Ralph is a 52 year old successful business man who comes into the office because of chronic fatigue and “just not feeling himself”. Over the years he was given a diagnosis of ADD, ADHD by his doctor who offered medication which Ralph declined. Left image of blood pressure cuff courtesy of AAFP.
Ralph has mild hypertension, and his doctors offered Ralph blood pressure pills for blood pressure of 145 over 95 mm Hg. Ralph declined the blood pressure pills, and instead takes supplements such as Magnesium and CoQ-10 and checks his BP at home daily with a home BP monitor. Examination reveals that Ralph is in good physical shape. He has good muscle tone from regular work outs at the gym, and is otherwise unremarkable.
Homozygous for MTHFR
Laboratory studies show that Ralph is homozygous for the MTHFR C667T mutation, and has elevated homocysteine. In addition to the basic protocol listed by Dr Ben Lynch (Basic Protocol for C667T (Click Here), Ralph was given Riboflavin (vitamin B2), a known treatment for hypertension in the MTHFR patient. Left Image courtesy of Stop the Thyroid Madness.
Methylation Pathways
How does Riboflavin, vitamin B2, work to reduce blood pressure? Riboflavin is an important co-factor in the methylation pathways, and has been found useful in reducing blood pressure in hypertension associated with homozygous MTHFR C667T . Riboflavin (vitamin B2) in the form of FAD acts as a cofactor for MTHFR.(1-2).
Riboflavin More Effective than AntiHypertensive Drugs
In her 2014 article, Dr Helen Mcnulty concludes:
“Thus riboflavin, targeted specifically at this genetically at-risk group, may offer a personalized non-drug approach to managing hypertension.”(2)
In her 2013 article, Dr Carol Wilson says:
“In conclusion, these results show that riboflavin supplementation targeted at hypertensive individuals with the MTHFR 677TT genotype can decrease BP more effectively than treatment with current antihypertensive drugs only and indicate the potential for a personalized approach to the management of hypertension in this genetically at-risk group.”(4)
The Homocysteine Connection
Dr Moat says in 2003 (13)
“Riboflavin (vitamin B2) is the precursor for FAD, the cofactor for methylenetetrahydrofolate reductase (MTHFR). MTHFR catalyzes the formation of 5-methyltetrahydrofolate, which acts as a methyl donor for homocysteine remethylation. Individuals with the MTHFR 677C3T mutation have increased plasma total homocysteine (tHcy) concentrations, particularly in association with low folate status. It has been proposed that riboflavin may act together with folate to lower plasma tHcy, particularly in individuals with the thermolabile MTHFR T variant.”(13)
Helene McNulty concludes in her 2006 article:
“Although previously overlooked, homocysteine is highly responsive to riboflavin, specifically in individuals with the MTHFR 677 TT genotype.”(14)
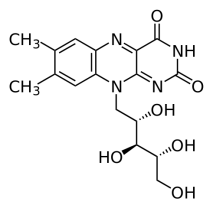 Riboflavin Deficiency caused by Oral Contraceptives
Riboflavin Deficiency caused by Oral Contraceptives
Studies show that birth control pills may cause riboflavin deficiency, thus aggravating clinical findings in the MTHFR patient. (15) Left image: Chemical Structure of riboflavin vitamin B2, courtesy of wikimedia commons.
Articles with related interest:
Blood Pressure Pills for Hypertension, When to Treat?
Fifty Million Americans have High Blood Pressure
Understanding Online Genetic Testing
Jeffrey Dach MD
7450 Griffin Road Suite 190
Davie, Fl 33314
954-792-4663
Links and references:
1) full pdf Riboflavin Lowers Blood Pressure Strain 2015
Strain, J. J., et al. “Riboflavin Lowers Blood Pressure: A Review of a Novel Gene-nutrient Interaction.” Nutrition and Food Sciences Research 2.2 (2015): 3-6.
full pdf
2) McNulty, Helene, J. J. Strain, and Mary Ward. ” Riboflavin lowers blood pressure in hypertensive people with the MTHFR 677TT genotype McNulty 2014 .” Archives of Public Health 72.Suppl 1 (2014): K2.
3) Shi, Zumin, et al. “Riboflavin intake and 5-year blood pressure change in Chinese adults: Interaction with hypertensive medication.” Food & Nutrition Bulletin 35.1 (2014): 33-42.
4) http://hyper.ahajournals.org/content/61/6/1302.full
Wilson, Carol P., et al. “Blood Pressure in Treated Hypertensive Individuals With the MTHFR 677TT Genotype Is Responsive to Intervention With Riboflavin Findings of a Targeted Randomized Trial.” Hypertension 61.6 (2013): 1302-1308.
Intervention with riboflavin was recently shown to produce genotype-specific lowering of blood pressure (BP) in patients with premature cardiovascular disease homozygous for the 677C→T polymorphism (TT genotype) in the gene encoding the enzyme methylenetetrahydrofolate reductase (MTHFR). Whether this effect is confined to patients with high-risk cardiovascular disease is unknown. The aim of this randomized trial, therefore, was to investigate the responsiveness of BP to riboflavin supplementation in hypertensive individuals with the TT genotype but without overt cardiovascular disease. From an available sample of 1427 patients with hypertension, we identified 157 with the MTHFR 677TT genotype, 91 of whom agreed to participate in the trial. Participants were stratified by systolic BP and randomized to receive placebo or riboflavin (1.6 mg/d) for 16 weeks. At baseline, despite being prescribed multiple classes of antihypertensive drugs, >60% of participants with this genotype had failed to reach goal BP (≤140/90 mm Hg). A significant improvement in the biomarker status of riboflavin was observed in response to intervention (P<0.001). Correspondingly, an overall treatment effect of 5.6±2.6 mm Hg (P=0.033) in systolic BP was observed, with pre- and postintervention values of 141.8±2.9 and 137.1±3.0 mm Hg (treatment group) and 143.5±3.0 and 144.3±3.1 mm Hg (placebo group), whereas the treatment effect in diastolic BP was not significant (P=0.291). In conclusion, these results show that riboflavin supplementation targeted at hypertensive individuals with the MTHFR 677TT genotype can decrease BP more effectively than treatment with current antihypertensive drugs only and indicate the potential for a personalized approach to the management of hypertension in this genetically at-risk group.
5) http://ajcn.nutrition.org/content/95/3/766.short
Wilson, Carol P., et al. “Riboflavin offers a targeted strategy for managing hypertension in patients with the MTHFR 677TT genotype: a 4-y follow-up.” The American journal of clinical nutrition 95.3 (2012): 766-772.
Optimizing riboflavin status offers a low-cost targeted strategy for managing elevated BP in this genetically at-risk group. These findings, if confirmed in the general population, could have important implications for the prevention of hypertension.
6) Wilson, C. P., et al. “Postgraduate Symposium The MTHFR C677T polymorphism, B-vitamins and blood pressure.” Proceedings of the Nutrition Society 69.01 (2010): 156-165.
7) Horigan, Geraldine, et al. “Riboflavin lowers blood pressure in cardiovascular disease patients homozygous for the 677C→ T polymorphism in MTHFR.” Journal of hypertension 28.3 (2010): 478-486.
8) Ward, Mary, et al. “B-vitamins, methylenetetrahydrofolate reductase (MTHFR) and hypertension.” International Journal for Vitamin and Nutrition Research 81.4 (2011): 240-244.
9) McCully, Kilmer S. “Homocysteine, vitamins, and vascular disease prevention.” The American journal of clinical nutrition 86.5 (2007): 1563S-1568S.
10) Lin, et al. “Low Plasma Pyridoxal 5’-phosphate Concentration and MTHFR 677C→ T Genotypes are Associated with Increased Risk of Hypertension.” International journal for vitamin and nutrition research 78.1 (2008): 33-40. Pyridoxal_5_phosphate_MTHFR_677C_Hypertension_Lin_2008
11) Durga, Jane, et al. “Folate and the methylenetetrahydrofolate reductase 677C→ T mutation correlate with cognitive performance.” Neurobiology of aging 27.2 (2006): 334-343.
=========================
12) Hustad, Steinar, et al. “Riboflavin as a determinant of plasma total homocysteine: effect modification by the methylenetetrahydrofolate reductase C677T polymorphism.” Clinical Chemistry 46.8 (2000): 1065-1071.
13) Moat, Stuart J., et al. “Effect of riboflavin status on the homocysteine-lowering effect of folate in relation to the MTHFR (C677T) genotype.” Clinical chemistry 49.2 (2003): 295-302. Riboflavin Homocysteine Folate MTHFR C677T Moat 2003
14) McNulty, Helene, et al. “Riboflavin lowers homocysteine in individuals homozygous for the MTHFR 677C→ T polymorphism.” Circulation 113.1 (2006): 74-80. Background— Meta-analyses predict that a 25% lowering of plasma homocysteine would reduce the risk of coronary heart disease by 11% to 16% and stroke by 19% to 24%. Individuals homozygous for the methylenetetrahydrofolate reductase (MTHFR) 677C→T polymorphism have reduced MTHFR enzyme activity resulting from the inappropriate loss of the riboflavin cofactor, but it is unknown whether their typically high homocysteine levels are responsive to improved riboflavin status.
Methods and Results— From a register of 680 healthy adults 18 to 65 years of age of known MTHFR 677C→T genotype, we identified 35 with the homozygous (TT) genotype and age-matched individuals with heterozygous (CT, n=26) or wild-type (CC, n=28) genotypes to participate in an intervention in which participants were randomized by genotype group to receive 1.6 mg/d riboflavin or placebo for a 12-week period. Supplementation increased riboflavin status to the same extent in all genotype groups (8% to 12% response in erythrocyte glutathione reductase activation coefficient; P<0.01 in each case). However, homocysteine responded only in the TT group, with levels decreasing by as much as 22% overall (from 16.1±1.5 to 12.5±0.8 μmol/L; P=0.003; n=32) and markedly so (by 40%) in those with lower riboflavin status at baseline (from 22.0±2.9 and 13.2±1.0 μmol/L; P=0.010; n=16). No homocysteine response was observed in the CC or CT groups despite being preselected for suboptimal riboflavin status.
Conclusions— Although previously overlooked, homocysteine is highly responsive to riboflavin, specifically in individuals with the MTHFR 677 TT genotype. Our findings might explain why this common polymorphism carries an increased risk of coronary heart disease in Europe but not in North America, where riboflavin fortification has existed for >50 years.
15) Newman, Leonard J., et al. “Riboflavin deficiency in women taking oral contraceptive agents.” The American journal of clinical nutrition 31.2 (1978): 247-249. Riboflavin deficiency oral contraceptive Newman 1978 Am J Clin Nutr
Jeffrey Dach MD
7450 Griffin Road Suite 190
Davie, Fl 33314
954-792-4663
www.jeffreydachmd.com
http://www.drdach.com
http://www.naturalmedicine101.com
http://www.bioidenticalhormones101.com
http://www.truemedmd.com
Disclaimer click here: http://www.drdach.com/wst_page20.html
The reader is advised to discuss the comments on these pages with his/her personal physicians and to only act upon the advice of his/her personal physician. Also note that concerning an answer which appears as an electronically posted question, I am NOT creating a physician — patient relationship. Although identities will remain confidential as much as possible, as I can not control the media, I can not take responsibility for any breaches of confidentiality that may occur.
Copyright (c) 2015 Jeffrey Dach MD All Rights Reserved. This article may be reproduced on the internet without permission, provided there is a link to this page and proper credit is given.
FAIR USE NOTICE: This site contains copyrighted material the use of which has not always been specifically authorized by the copyright owner. We are making such material available in our efforts to advance understanding of issues of significance. We believe this constitutes a ‘fair use’ of any such copyrighted material as provided for in section 107 of the US Copyright Law. In accordance with Title 17 U.S.C. Section 107, the material on this site is distributed without profit to those who have expressed a prior interest in receiving the included information for research and educational purposes.
Serving Areas of: Hollywood, Aventura, Miami, Fort Lauderdale, Pembroke Pines, Miramar, Davie, Coral Springs, Cooper City, Sunshine Ranches, Hallandale, Surfside, Miami Beach, Sunny Isles, Normandy Isles, Coral Gables, Hialeah, Golden Beach ,Kendall,sunrise, coral springs, parkland,pompano, boca raton, palm beach, weston, dania beach, tamarac, oakland park, boynton beach, delray,lake worth,wellington,plantation.
The post Riboflavin for Hypertension in MTHFR appeared first on Jeffrey Dach MD .










Leave a Comment
You must be logged in to post a comment.