 Pantothenic Acid, Vitamin B5 for Acne
Pantothenic Acid, Vitamin B5 for Acneby Jeffrey Dach MD
Virtually everyone remembers the frustrating experience of acne with small inflamed dots called pimples or blackheads. While some have been spared the ordeal of acne, many others have suffered through unsuccessful treatments over years in spite of the best efforts of top dermatologists. Although some of the treatments (such as Accutane) may be successful, they come at the price of serious adverse side effects such as depression.
Left Image: Mona Lisa with Acne, Courtesy of Leonardo DaVinci on Wikimedia Commons.
For the young woman concerned about self-image, skin complexion is obviously very important. Even a small amount of acne with one or two strategically placed pimples can be intolerable. For the unfortunate few, acne can be progressive leading to scarring and disfigurement, with the pitting and nodularity of Acne Vulgaris.
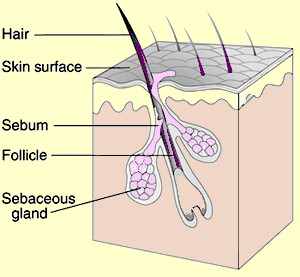
Note Sebum (pink) in this diagram of hair follicle with sebaceous glands and sebum (pink). Courtesy of Wikimedia Commons
Acne is caused by excess oil in the skin (also known as sebum). This oil comes from sebum secretion by the sebaceous glands at the root of the hair follicles. This oily build up occludes the pores in the skin causing blockage and infection. The well known practice of “popping” the pimple forces the occluding plug to pop out of the pore, thereby allowing drainage of the sebaceous glands at the root of the hair follicle and providing temporary relief.
Acne is a common adverse side effect of synthetic birth control pills which mimic testosterone. Elevated testosterone levels in males and females are associated with increased oil production in the skin resulting in acne. A common genetic mutation called atypical CAH (congenital adrenal hyperplasia) causes increased testosterone in females resulting in acne. PCOS (polycystic ovary syndrome) syndrome is associated with increased testosterone production and acne is common.
Young males may suffer from acne merely because of abundant (and normal) testosterone production. Below, we will make the case for a vitamin B5 deficiency as a cause for acne.
Traditionally, acne is treated by the dermatologist with various topical cleansers, antibiotics and drugs such as Accutane. Accutane’s most commonly reported adverse side effect is depression which can lead to suicide.
In this article we will present to you information about Vitamin B5 (pantothenic acid) as a treatment for acne. We will explain the role of Vitamin B5 in the metabolism of fats and oils, and how increasing the metabolism of oils will reduce oil accumulation in the skin, and thereby reduce or eliminate acne. Both Accutane and Vitamin B5 work by different mechanisms. Accutane works by shrinking the sebaceous glands at the root of the hair follicles. However, Vitamin B5 works by reducing the oil production of the sebaceous glands. This is done by increasing Coenzyme A (Co-A) which increases the metabolic breakdown of oils by normal activity of cell physiology.
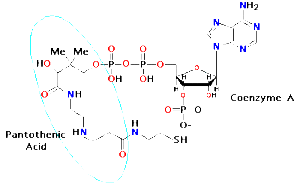
I first became aware of the use of Vitamin B5 (also called pantothenic acid) as a treatment for acne from an article by Lit-Hung Leung (1997). In this article, Dr Leung explains that acne can be reduced or eliminated with the use of Vitamin B5, also called pantothenic acid.
Pantothenic acid is a major component of Co Enzyme A (see diagram above). CoA is used at the cellular level for fatty acid oxidation and in many other biochemical reactions in the cell. Taking additional B5 increases the amount of Coenzyme A available for use in the cell. The more Co-Enzyme A, the more fatty acids can be metabolized, which means they are oxidized or burned up as energy production.
CoEnzyme A is actually a Pantothenic Acid molecule attached to an ADP molecule (see diagram above, ADP=adenine triphosphate). ADP is widely available throughout cellular biochemistry as the currency of energy in the cell.
Pantethine is made of two Vitamin B5 molecules linked together with two sulfurs (S) in the center (see below diagram).
Pantethine Courtesy of Wikimedia Commons Note two B5, Pantothenic Acid Molecules attached with the two sulfur molecules (S) in the center.
It is well known that the Beta Oxidation of Fatty Acids depends on CoA. If there is a deficiency of Acetyl CoA in the body, oxidation of fatty acids will slow down, and the skin becomes oily resulting in acne. Increasing the amount of Acetyl CoA available speeds up the metabolism of fatty acids which are then used for energy production. Taking the vitamin B5, pantothenic acid is the easiest way to increase acetyl Co A and increase rate of fatty acid metabolism.
Dr. Leung gave his acne patients rather large doses of 5-10 grams of Pantothenic Acid a day with considerable improvement in their acne. He reported success with this regimen.
 Message Board Discuss Pantethine and B5 for Acne
Message Board Discuss Pantethine and B5 for AcneAfter reading Dr. Leung’s article, I then did a Google search for acne and B5, and found a large amount of information on message boards posted by people suffering from acne trying various treatments including pantothenic acid. I found that many, but not all, of these acne sufferers had success with vitamin B5 (Pantethine) which did work for many of them. However, a common complaint was that the large amount of pantethine (10 grams) was hard to take, causing gastrointestinal gas and bloating etc.
Obviously, the major difficulty with Dr Leung’s Vitamin B5 protocol is the large amount of B5 required. It would be advantageous to reduce the B5 dosage to a more reasonable level. Considering the biochemical pathways involved, this would be possible with the addition of L-carnitine, which transports fatty acids across the mitochondrial membrane where they can be oxidized.
According to the biochemistry of fatty acid oxidation, “Transport is RATE LIMITING STEP for oxidation of long chain fatty acids.” (1,2)
See the diagram below which shows the importance of L-Carnitine in transporting the fatty acid (the Acyl Group is the fatty acid chain) into the mitochondrial matrix.(1,2)
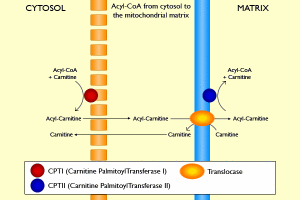
Above diagram courtesy of wikipedia showing L-Carnitine transporting fatty acids into the mitochondria where they can be oxidized. Carnitine transports long-chain acyl groups from fatty acids (Acyl group) into the mitochondrial matrix, so that they can be broken down through β-oxidation to acetate to obtain usable energy via the citric acid cycle.
Using the modified Leung B5 protocol with Pantethine 750 mg with 250 mg of L Carnitine three times a day, we have noted excellent success rates in reducing or eliminating acne. An added advantage is a good cosmetic result with smaller pore size and smoother skin. The vitamins are safe with no adverse side effects noted.
A college student under my care was making preparations for her upcoming wedding when she noticed some new acne lesions on her face. We immediately began the Pantethine and L-Carnitine. Her acne cleared up immediately, and she was quite pleased. By now, we have a number of satisfied patients who have used this program to clear up acne. I myself have used the program and can report that it works quite well.
Also Used for Weight Loss
Since this anti-acne regimen is essentially a fat burning protocol, it is also useful for weight loss.
No Adverse Side Effects
Unlike Accutane which may have serious adverse side effects. vitamin B5 have little or no adverse side effects.
Acetyl CoA is the first step in the body’s synthesis of Cholesterol. Cholesterol is then used to make all steroidal hormones. Many of the steroidal hormones are made by the adrenal gland, so it is very logical that B5 deficiency can result in a syndromes called adrenal failure, or the inability to synthesis steroidal hormones such as Cortisol. See my previous article on Adrenal Fatigue for more information about this syndrome.
Online Supplement Store:
Buy B5 Pantethine Here.
Buy L-Carnitine Here.
————————————————————————————–
 For example, there is a well know tendency for lupus to flare up under certain conditions in which there is a greater demand for steroidal hormone biosynthesis, such as puberty, and pregnancy. Females are more affected than males by a ratio of ten to one. Lupus preferentially affects females because they have greater demands for hormone production than do males. These lupus flares seem to correlate with demand for higher levels of hormones. Production of higher hormone levels could deplete the stores of precursor molecules for production of these hormones. The first such precursor molecule is acetyl CoA, so a deficiency in acetyl CoA could be the culprit.
For example, there is a well know tendency for lupus to flare up under certain conditions in which there is a greater demand for steroidal hormone biosynthesis, such as puberty, and pregnancy. Females are more affected than males by a ratio of ten to one. Lupus preferentially affects females because they have greater demands for hormone production than do males. These lupus flares seem to correlate with demand for higher levels of hormones. Production of higher hormone levels could deplete the stores of precursor molecules for production of these hormones. The first such precursor molecule is acetyl CoA, so a deficiency in acetyl CoA could be the culprit.
Another feature of female lupus patients is that when hormone levels are measured, they tend to run low. Irregular menstrual cycles and absent menses is common among lupus patients. Giving hormones to raise levels seems to help.
For example, Quality of Life for Lupus patients seems to be ameliorated by DHEA administration, an adrenal hormone precursor. DHEA administration can even reduce the number of Lupus Flares.
After menopause when hormone production declines dramatically, there is a reduction in Lupus flares and the disease becomes quiescent.
Acne tends to be a common issue for lupus patients given DHEA, and this would be expected assuming there is an underlying B5/Acetyl CoA deficiency. Administration of B5 along with the DHEA usually resolves the acne.
Cortisol production is also decreased in lupus patients, explaining why they do better when treated with steroids.
Another interesting feature of Lupus is that the disease can be caused by 70 various drugs. The three most common are procainamide, hydralazine and isoniazid. These drugs have nothing in common except they are metabolized by the acetylation pathway, a connection to Acetyl CoA.
The first manifestations of Deficiency States are in the skin, joint and connective tissue with various lesions. The vital organs are only involved much later on. For example, deficiency states such as beri beri and scurvy initially spare the vital organs, and involve the skin and musculoskeletal system. Lupus follows this pattern as well.
In his article, Dr. Leung noted a connection between Systemic Lupus (SLE) and Acetyl CoA deficiency, however he was not the first to suggest giving Pantethine (Vitamin B5) to Lupus patients. There were a number of reports on this in the 1950’s. However, early studies seemed to discredit the whole idea of B5 deficiency or acetyl CoA deficiency or a genetic acetylation defect in Lupus. Nonetheless, Leung reported improvement in his lupus patient who supplemented with pantothenic acid. Late stages of Lupus are characterized by specific anti nuclear antibodies (ANA test) which obviously will not be affected by giving pantothenic acid.
However, much can be done to improve quality of life of the lupus patient. Perhaps a combined approach supplementing with bioidentical hormones such as estradiol, progesterone, DHEA, Cortef, testosterone as well as vitamin mineral supplementation with pantethine, and others would be the most logical way to help lupus patients get back their health.
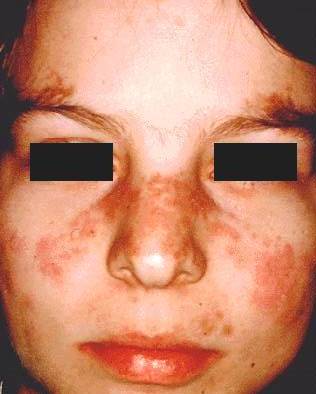
Another interesting connection is the appearance of a skin rash on the face in lupus flares with pregnancy. There can be increased facial skin pigmentation in pregnancy itself (without lupus) called Melasma, also known as chloasma or the mask of pregnancy. Also, Addisons Disease, adrenal failure, or failure to produce sufficient adrenal hormones results in hyper-pigmentation changes in the face and elsewhere. Characteristic sites are skin creases in the hands, and the inside of the cheek (buccal mucosa), also old scars may darken.
All three, Lupus, Prognancy and Addisons, share the same mechanism, the need to stimulate more adrenal steroidal hormone synthesis by increasing ACTH levels (ACTH = adreno cortico stimulating hormone). ACTH is secreted by the pituitary to stimulate more adrenal hormone synthesis. Increased ACTH also causes an increase in melanocyte-stimulating hormone (MSH). The melanocytes cause the pigmentation.
A 45 year old lupus patient came to see me in the office. She had been to many rheumatologists and specialists over the years with a confirmed diagnosis of lupus. She appeared under weight and chronically ill, and had absent menses for the last 7 years. Her main complaint was severe chronic fatigue and inability to gain weight. In the past she had been on many of the usual drug treatments for lupus with many adverse effects and no real improvement in quality of life.
Initial testing showed low salivary cortisol, and low serum levels for the other hormones, DHEA, estradiol, progesteron and testosterone. She also had low B12 and Vitamin D levels. She was started on bio-identical hormones, Pantethine (B5), B12 and Vitamin D. About three months after starting treatment, she calls me and states she is feeling much better with improved energy levels, and she just had a normal period, the first one after seven years of absent menses.
For more information on the use of B5, Pantothenic Acid and Adrenal Fatigue, see my previous article: Adrenal Fatigue by Jeffrey Dach MD
Online Supplement Store:
Buy B5 Pantethine Here.
Buy L-Carnitine Here.
Update 2014:
Vitamins_for_Treatment_of_Cutaneous_Disorders_Andrea_Chiricozzi_JNT_2013
Jeffrey Dach MD
www.jeffreydach.com
www.drdach.com
www.naturalmedicine101.com
www.truemedmd.com
Links and References
1) http://www.ncbi.nlm.nih.gov/pubmed/15590999/
Ann N Y Acad Sci. 2004 Nov;1033:1-16.
The role of the carnitine system in human metabolism.
Foster . Metabolism cycles daily between the fed and fasted states. The pathways of energy production are reversible and distinct. In the anabolic (fed) state, the liver stores glucose as glycogen, and fatty acid/triglyceride synthesis is active. In the catabolic (fasted) state, the liver becomes a glucose producer, lipogenesis is slowed, and fatty acid oxidation/ketogenesis is activated. The rate-limiting step for the latter is vested in the carnitine/carnitine palmitoyltransferase (CPT) system, and the off/on regulator of this is malonyl CoA. The AMP-induced protein kinase primarily determines the concentration of malonyl CoA. Four other systems have significant influence: two on fatty acid oxidation and two on lipogenesis. Peroxisome proliferator-activated receptor gamma-1 alpha, a master regulator of metabolism, induces hepatic gluconeogenesis and fatty acid oxidation in the catabolic phase. Deficiency of stearoyl CoA desaturase, although having no role in gluconeogenesis, powerfully induces fatty acid oxidation and weight loss despite increased food intake in rodents. Major stimulators of lipogenesis are carbohydrate-responsive element binding protein and the Insig system. The malonyl CoA-regulated CPT system has been firmly established in humans. The other systems have not yet been confirmed in humans, but likely are active there as well. Activation of fatty acid oxidation has considerable clinical promise for the treatment of obesity, type 2 diabetes, steatohepatitis, and lipotoxic damage to the heart.
2) http://www.ncbi.nlm.nih.gov/pubmed/10856709
Biochim Biophys Acta. 2000 Jun 26;1486(1):1-17.
Fatty acid import into mitochondria.Kerner J1, Hoppel C.
3) http://www.vilantae.com/index.php
Vilante Home, and Video
4) http://www.b5acnetreatment.com/2007_03_01_archive.html
Vilante B5 web site
http://www.acnetohealth.com/vitamin-b-5-acne.html
The Vitamin B 5 Acne Theory Debunked
http://forum.lef.org//default.aspx?f=35&m=22990
message board LEF
http://deficiencydiseases.com/
Papers by Lit-Hung Leung, M.D.
http://www.coenzyme-a.com/acne_vulgaris.html
Pantothenic Acid in the Treatment of Acne Vulgaris
“A Medical Hypothesis” by Lit-Hung Leung, M.D.
The Effect of Pantothenic Acid on Acne Vulgaris
One hundred patients of Chinese descent were included in the study, 45 males and 55 females. The age ranged from 10 to 30, and with about 80% between 13 and 23. The severity of the disease process varied. They were given 10 grams of pantothenic acid a day in four divided doses.
To enhance the effect, the patients were also asked to apply a cream consisting of 20% by weight of pantothenic acid to the affected area, four to six tines a day. With this treatment regimen, the response is as prompt as it is impressive.
There is a noticeable decrease in sebum secretion on the face usually 2-3 days after initiation of therapy. The face becomes less oily.
After two weeks, existing lesions start to regress while the rate of eruption of new acne lesions begins to slow down.
In cases with moderate severity, the condition is normally in complete control in about eight weeks, with most of the lesions gone and new lesions only to erupt occasionally.
In those patients with severe acne lesions, complete control may take months, sometimes up to six months or longer.
In some of these cases, in order to get a more immediate response, it may even be necessary to step up the dose to 15-20 grams a day. In any event, the improvement is normally a gradual and steady process, with perhaps minor interruptions by premenstrual flare or excessive intakes of oily food. With this form of treatment, another striking feature is the size of the facial skin pore.
The pore size becomes noticeably smaller within one to two weeks, very often much sooner. Like sebum excretion, the pores will continue to shrink until the skin becomes much finer, giving the patient a much more beautiful skin.
This decrease in skin pore size is presumably related to sebum excretion. When an acne lesion is formed, there is in the epithelial cell of the hair follicle an accumulation of lipids, leaving the epithelial cells bulky and the lumen of the gland narrowed. When there is a concomitant increase in sebum flow, the follicle has no choice but to hypertrophy to accommodate the changes, resulting in an enlarged skin pore and coarse skin. With the administration of pantothenic acid, the whole process is reversed. Lipid metabolism becomes normal and efficient. The epithelium is no longer laden with fat droplets, there is a decrease in sebum excretion, the hypertrophy process is not required. The skin pores revert to a much smaller size and the skin becomes smooth and fine.
As acne lesions tend to subside spontaneously after puberty, some patients do not need a maintenance dose. But, if a patient is in his mid-teens, when the sexual characteristics have yet to fully develop, it may be necessary for replacement therapy to be implemented. This maintenance dose, can be lowered, or increased with the clinical symptoms. A maintenance dose will not only act as a preventive measure against sporadic eruption, but the extra pantothenic acid will help to ease the relative deficiency state, and likely improve the general health of the patient.
http://www.coenzyme-a.com/research.html
Research Articles on Coenzyme A
http://www.coenzyme-a.com/research.html
The following is an excerpt from the article,
Pantethine: A Review of their Biochemistry and Therapeutic Applications
first published in Alternative Medicine Review, Volume 2, Number 5.
http://www.coenzyme-a.com/research.html
Pantothenic Acid in the Treatment of Obesity
“A Medical Hypothesis” by Lit-Hung Leung, M.D.
This article originally appeared in the scientifically prestigious Journal of Orthromolecular Medicine Vol. 12 Number 2, 1997. The version below is from a reprint of the original article.
http://www.coenzyme-a.com/research.html
Coenzyme-ATM “Precursor The Master CoenzymeTM”
by Nickolaos D. Skouras, Ph.D.
http://www.acne.org/messageboard/index.php?showtopic=15341
Acne.Org message board…nuts and bolts advice on b5
Very Good Summary
http://www.ironmagazineforums.com/history/topic/23051-1.html
acne b5 accutane message board
http://www.getmyarticles.com/articles/Social_Issues/Who_Is_Dr._Lit_hung_Leung__122154.html
http://www.clearskin.net/viewtopic.php?t=1907
Very extensive discussion of B5 on message board
ClearSkin.net. Also contains email correspondence with Dr Leung
Here is a brief summary of my own B5 use: by William G. Gray
• Started November 10th at 5 grams per day
• After noticeable acne clearing, increased dosage after 1 week to 10 grams per day
• After another 2 weeks of more dramatic improvements, increased dosage to 15 grams per day, and maintained daily dosage to present
I spread my B5 intake over the day, divided into 6 x 2.5 gram doses. I’ve found the B5 seems more effective if I don’t take it with food, but rather take it at least 10-15 minutes before a meal or at least an hour afterward. I currently use TwinLab brand, 500mg B5 capsules.
My improvements have been that I now get virtually no acne…except if I eat a lot of sugary and/or oily food, in which case the few acne bumps I do get are extremely minor and disappear quickly, never getting infected. My skin is still slightly oily from the seborrheic dermatitis, but it is no longer as red and irritated as it used to be, and the dermatitis seems to be gradually fading.
The only negative side effects I noticed were minor diarrhea at first, accompanied by hunger cravings, both of which disappeared after a few days (the diarrhea after about 2). I did notice the diarrhea effect again when I increased my dosages, but it again disappeared after a couple of days.
I have noticed at least two positive side effects: increased energy throughout the day, and what seems to be a boost to my immune system; I have been exposed to all manner of colds, flu, and illness this winter and have not gotten sick, whereas normally I would have gotten at least a couple of colds.
Sincerely,
William G. Gray
http://b5foracne.vze.com/
B5 For Acne Web Site
http://b5foracne.vze.com/
Very well organized testimonials area with photos STUDY Pantothenic Acid (b5) and Acne Study by Dr Leung
http://www.acnemiracle.com/home.html
Acne Miracle popular merchants of b5 powder and topical b5. Site also contains info about b5
http://gmuntz.tripod.com/b5.html
Natural Acne Treatments
http://www.vitaminb5acne.com/faq.html
Vitamin B5 for Acne
http://orthomolecular.org/library/jom/1997/articles/1997-v12n02-p099.shtml
The Journal of Orthomolecular Medicine Vol. 12, 2nd Quarter 1997
A Stone that Kills two Birds: How Pantothenic Acid Unveils the Mysteries of Acne Vulgaris and Obesity Lit-Hung Leung. M.D.
http://deficiencydiseases.com/
articles by Lit-Hung Leung
http://deficiencydiseases.com/SLE_full_text.pdf
LUPUS ERYTHEMATOSUS: A COMBINED DEFICIENCY DISEASE Lit-Hung Leung, M.D. Formerly Consultant Surgeon, Department of General Surgery, Hong Kong Central Hospital, Hong Kong.
http://orthomolecular.org/library/jom/1997/pdf/1997-v12n02-p099.pdf
A Stone that Kills two Birds: How Pantothenic Acid Unveils the Mysteries of Acne Vulgaris and Obesity… LH Leung – Journal of Orthomolecular Medicine, 1997 – orthomolecular.org
It has been hypothesized that acne vulgaris is linked to Coenzyme-A due to its activity in fatty acid metabolism and sex hormone synthesis (Lit-Hung Leung, M.D., Pantothenic Acid in the Treatment of Acne Vulgaris, “A Medical Hypothesis” , Journal of Orthromolecular Medicine Vol. 12, No. 2, (1997)). Coenzyme-A is formed from adenosine triphosphate, cysteine and Pantothenic Acid. A deficiency in Pantothenic Acid potentially inhibits or reduces the activity of Coenzyme-A in its fatty acid metabolism and sex hormone synthesis. If the fatty acid metabolism activity is diminished, lipids, which are a combination of fatty acids, begin to accumulate in the sebaceous glands thereby increasing the sebum excretion and in turn, the production of acne vulgaris. Pantothenic Acid is essential for the proper functioning of Coenzyme-A and its related activity; if a deficiency in Pantothenic Acid exists, an increase of sebum production occurs due to the accumulation of lipids in the sebaceous glands. Pantothenic Acid in the present invention therefore reduces sebum production.
http://www.ncbi.nlm.nih.gov/pubmed/7476595?dopt=Abstract
Med Hypotheses. 1995 Jun;44(6):490-2.
Pantothenic acid deficiency as the pathogenesis of acne vulgaris.
Leung LH.
Department of General Surgery, Hong Kong Central Hospital, Hong Kong.
For years, the pathogenesis of acne vulgaris has been known to be strongly influenced by hormonal factors. However, the exact role of and the interrelationship among the various hormones in question have not been well elucidated. Here, I wish to suggest a radically different theory for its pathogenesis and relate its basic pathology to a deficiency in pantothenic acid, a vitamin hitherto not known to cause any deficiency syndrome in humans. Hence, the effect of hormonal factors in this disease entity becomes secondary to that of the availability of pantothenic acid. A complete cure of this condition is effected by a very liberal replacement therapy with the vitamin.
http://ezinearticles.com/?Using-Pantothenic-Acid-(Vitamin-B5)-as-an-Acne-Treatment&id=48855
Using Pantothenic Acid (Vitamin B5) as an Acne Treatment By Ryan Bauer
http://www.ncbi.nlm.nih.gov/pubmed/3976557?dopt=Abstract
Am J Clin Nutr. 1985 Mar;41(3):578-89.Related Articles, Links
Effects of supplemental pantothenic acid on wound healing: experimental study in rabbit.
Aprahamian M, Dentinger A, Stock-Damgé C, Kouassi JC, Grenier JF.
These data suggest that pantothenic acid induces an accelerating effect of the normal healing process.
http://lpi.oregonstate.edu/infocenter/vitamins/pa/
Pantothenic Acid
http://askwaltstollmd.com/archives/acne/71477.html#72393
Acne Archives Pantothenic Acid’s (possible) Bad Side
http://www.bastyrcenter.org/content/view/439/
Nutritional Supplements In The Treatment Of Acne
Scientific evidence suggests that nutritional supplements may be useful treatments for acne, a common and embarrassing skin condition that afflicts both adults and teenagers. Increased stimulation of the skin and bacterial infections appear to play major roles in the development of acne. Conventional treatments include drying agents, topical anti-inflammatory medications, antibiotics and, in severe cases, steroids. While prescription medications may be effective, many of these substances have side effects that limit the duration of use. Some studies suggest that certain natural oral and topical treatments may work as well as prescription medications, with fewer reported side effects.
Several studies have shown that taking zinc may reduce the severity of acne.1 2 Most of the studies used 50 mg of zinc three times per day. However, with the development of better absorbed forms of zinc, many doctors now recommend 30 mg two or three times per day initially, and lower amounts after the first 12 weeks. One study found that zinc may be as effective as oral antibiotic therapy.3 It is recommended to take zinc with food to avoid getting an upset stomach. Long-term use of zinc may require adding 1 to 2 mg per day of copper to prevent copper deficiency.
The results of another study suggest that vitamin B5 (pantothenic acid) may also be useful in treating acne.4 However, participants in the study took 10 grams per day orally, which is an extremely large amount, and also used a 20% topical cream of vitamin B5 daily. Although no significant side effects occurred, the long-term safety of such large amounts taken orally has not been studied. Mild cases cleared in a couple of months and more severe cases took up to six months to clear. It is unknown whether lower amounts would produce the same results.
In another study, high amounts of vitamin A were used to treat severe acne in teenagers.5 Girls took up to 300,000 IU per day and boys took up to 500,000 IU per day. Although the acne was lessened, the benefit seemed to diminish once the oral vitamin A therapy was discontinued. Such high intake is potentially toxic and should only be done under the supervision of a physician.
Women with premenstrual acne may find benefit with vitamin B6. One small trial found 50 mg per day of vitamin B6 (pyridoxine) alleviated flare-ups of acne before the onset of their menstrual cycles.6
Using topical formulations may help with acne as well. One study showed that a 4% niacinamide gel used twice daily for two months significantly reduced acne lesions.7 Other trials have demonstrated that a 20% azelaic acid cream worked as well as benzoyl peroxide, oral tetracycline and retinoic acid.8 9 Although these topical formulas are natural substances, they are available only by prescription.
For more information on herbal therapies for acne, see today’s related Newswire article.
References:
1. Hillström L, Petterson L, Hellbe L, et al. Comparison of oral treatment with zinc sulfate and placebo in acne vulgaris. Br J Dermatol 1977;97:681–4.
2. Verma KC, Saini AS, Dhamija SK. Oral zinc sulphate therapy in acne vulgaris: a double-blind trial. Acta Derm Venereol 1980;60:337–40.
3. Michaelsson G, Juhlin L, Ljunghall K. A double blind study on the effect of zinc and oxytetracycline in acne vulgaris. Br J Dermatol 1977;97:561–6.
4. Leung LH. Pantothenic acid deficiency as the pathogenesis of acne vulgaris. Med Hypotheses 1995;44:490–2.
5. Kligman AM, Mills OH Jr., Leyden JJ, et al. Oral vitamin A in acne vulgaris. Preliminary report. Int J Dermatol 1981;20:278–85.
6. Snider B, Dietman DF. Pyridoxine therapy for premenstrual acne flare. Arch Dermatol 1974;110:130–1[letter].
7. Shalita AR, Smith JR, Parish LC, et al. Topical nicotinamide compared with clindamycin gel in the treatment of inflammatory acne vulgaris. Int J Dermatol 1995;34:434–7.
8. Nazzaro-Porro M. Azelaic acid. J Am Acad Dermatol 1987;17:1033–41.
9. Norris J. Azelaic acid really does work in acne—a double blind national and international study. Br J Dermatol 1987;32(Suppl):34.
http://www.dermatologytimes.com/dermatologytimes/article/articleDetail.jsp?id=188762
• Vitamin A acetate 5000 IU
• Vitamin E succinate 400 IU
• Vitamin B-6 50 mg
• Pantothenic acid 500 mg
• Zinc methionine 50 mg
• Selenium (L-selenomethionine) 200 μg
• Chromium polynicotinate 200 μg
• Barberry root bark xpowder (berberine) 500 mg
Pantethine:
http://www.acne.org/messageboard/index.php?showtopic=21524&st=60
i personally think it is crazy to take 10 grams of something to try and rid acne. I don’t think its crazy to try and rid acne (cause i would do anything to get rid of it), but taking such high doses doesn’t seem very smart.
After reading about pantethine (the active form of B-5), i’m wondering why people aren’t trying it instead of b5? From what ive read, you get a better effect with a lot less to no side effects. Because you only have to take around 900 mg or so of pantethine, there will be no adverse side effects.
Has anyone tried pantethine that had no success with b5? or if you never used b5 but are having success with pantethine please share. I’m just curious as to why people are using this supplement that seems like a much healthier avenue than b5
—-
I can’t agree with you more, I am currently taking pantethine instead of B5 only at 300mg. 300mg for me is equivalent to about 6grams of B5.
I just don’t see the sense in taking so many pills at such a high strength when I get better results using pantethine at a lower dosage. I can’t say enough about how this product has worked for me. Although it appears that after searching this board, hardly anybody uses it.
——
I have been using pantethine for about 2 years now. I started taking B5 in january of 2001 and quit later in 2002. I always found that B5 for me wasn’t as effective as taking pantethine, although I didn’t have any side effects, like hair loss that some have. my skin is definitely alot drier now. When I started taking pantethine, I started at 600 mg and included 2G of B5, but I gradually over the course of a year cut down to 300mg per day and stopped B5, and I also take 50mg of zinc and a multivitamin too, but I was also doing that when I taking B5. I tried it once for a week at 900mg, and my skin was way too dry, so I had to cut down. I have used couple different brands and had success with all of them. The cheapest that I can find is using a brand call NOW; it’s only about $11-12 for 60 softgels. I was using Jarrow, but they were too expensive, $18-$19.
If you want to try it, try and include a 450mg or 300mg pill and gradually diminish your B5 dosage over time. Play around with dosage and see what works best for you, that’s what I did. This is so much better than trying to swallow 6-7 1G giant B5 pills.
==============
malia, I first heard about pantethine on another site www.healthboards.com. I first learned of B5 in late 2000 when it was hardly known to be so beneficial, so I tried it (B5), and I couldn’t believe the effects that it gave me. adding that and zinc into my routine definitely helped me to control the problem. But after several months, I came across a post on healthboards.com of a person who was using both pantethine and B5 and claimed that adding panthetine improved his skin more. Then I had only minor breakouts from taking B5 regularly, so I bought some and took B5 and pantethine together for quite some time, and it definitely had more of a beneficial effect. Like I said, my skin became much drier. somehow, it seemed as though my body was using the pantethine more readily than B5. Because now, 300 or 600mg per day for me is equivalent to 6-8g of B5. I now only wish I had discovered B5 and pantethine earlier in my life like when I was in high school. I was also always concerned about the megadosing of the vitamin too.
for the three of you: malia, 2SG, and dude123, I wouldn’t stop taking B5 when you get your order, definitely take both for some time and diminish B5 accordingly.
————–
just to update you on my pantethine supplement, I have definitely noticed less oil on my forehead….It used to become very oily between my eyes, and normally I always had a blemish there, but it is definitely becoming less and less…..I did not see this difference using B5 for 2.5 months either
============
I’ve been waiting to post until I had something to say…..anyway, I’ve been takin B-5 for about 3wks (over 2 years ago I took about 5 Grams per day for a month or two and my acne cleared all up But then I started trying to concieve and didn’t want to take any chances)
Now that I am finished Breast feeding I started 5 grams again, but then I read about Pantethine and have been taking that for the last week. So far there has been no complications from switching from b-5 to pantethine (900mg). My face looks great. No new break outs after the initial breakout beginning the first week of taking the b-5. I can tell my skin is much dryer and my lips are a tad dryer, I’ve been needing to use carmex on them. My hands need lotion too.
Between Pantethine and Dan’s BP GEL I look and feel great!! I think this is really promising!!
(moderate a
——————
Hi Malia, I switched from 5 grams of b-5 to Pantethine one week ago today. I can’t tell the difference, only less pills to take. I was taking 10 pills and now I’m only taking 3 small soft gels Pantethine.
I’m using the NOW brand of Pantethine. It cost 22.49 (usd) at my local healthfood store. No new breakouts!! I know it’s working because I’ve got to use Carmex on my lips and have a little bit dryer hands. I’m still not completely oil free on my face, but I can tell it’s much less and my face is clear.
So far so good. I’m really happy about this prospect!!
(to be fair I’ve always been on BP, for the last 15 yrs and it’s always helped my face, but I’ve never been clear always about 3 or more spots in one day. I don’t follow Dan’s routine. But I do believe in his BP Gel. I don’t eat very well, I have hormonal acne and I only wash my face when I take a shower, which is every two days because the ends of my hair tend to be dry! And I switched from Neutrogena’s BP to Dan’s 3 days ago! I only put it on at night before I go to bed.)
———————
I have come to the conclusion that there is not difference between pantithine and panothenic acid mg vs mg. If you are taking only 900mg of pantithine as opposed to 5-10g, of panothenic acid your are not fooling your skin. I don’t know who made the false claims that pantithine is stronger then panothenic acid. Its exactly the same in my opinion from using it for the last 2 months. Don’t waste your time with pantithine because it cost more and does exactly the same.
————————-
I take 300 mg of Pantethine, 3 times a day, so 900mg total. It works the same as megadosing on B5. And it’s safer, you don’t have to take so many B5 pills. I heard that you can get calcium buildup in your kidney if you take B5 megadose for a long time. It’s dangerous. A person had to get a painful kidney stone removed because of the calcium buildup from megadosing on B5.
Pantethine is safer and works the same. It is the active ingredient in Vitamin B5. If you have -any questions, feel free to ask me and I’ll respond in this thread.
——
Jul 16 2007, 12:44 PM
guys,
I wish I had seen the info on pantethine before starting b5 powder 10 days ago. I have had moderate acne for 30 years… had 4 rounds of accutane. Currently on minocycline, tazorac, 2.5% benzoyl peroxide. This minimized my acne to 2-3 small lesions at any time.
So far, the b5 is affecting my skin AS WELL AS accutane. My oil slick of a face is almost at normal sebum levels already. My nose isn’t shiny after all day at work. I’m excited, because if I can back off the dosage after 3 months, it could be a maintenance drug!!! No more oily skin and zits!
I think I’ll maintain the b5 and watch for posts from people who have switched over to the pantethine.
BTW: I am an inorganic chemist and medical researcher. This stuff is not without side effects (diarrhea-common, hair loss-rare). From what I’ve read, you need to take a multi-b vitamin while megadosing b5. Since it’s water soluble (not fat soluble) the excess will be excreted from your body. Compared to accutane (stores in the liver) risks are minor.
Good luck!!!!
_____________________
Aug 13 2007, 01:25 AM
K so I started taking Pantethine for my acne last month with a B-complex daily, was on 1200 MG’s each day spread into 3 pills, usually around 5-6 hours apart, 450/450/300. after about 3 days i noticed my skin a hella lot less oily, but then it seem’d to slowly return at around day 5, i experince a pretty lame breakout after a few days that got a little worse up untill about 2 weeks, at about 2 weeks i started to see MINOR results i might be wrong …. anyways im a little over a month now and i have barely NO acne anymore, i didn’t really notice at first but now that i look its al lred spots now theres NO acne, and my skin is looking fresher then FREAKING EVER. Pantethine owned all the little zits right away and then slowly *dried up* all other larger white heads. Now when i feel my face it feels smooth and im LOVING it, only continue’ing to get better too im still getting 1 major pimple each week but thety get owned QUICK LOL so yea, IM A BELIEVER, PATETHINE = OWNAGE gonna post my next update sometime in a few more weeks I hope it keeps working gonna alsp try some acv for my red spots see how that goes … PEOPLE USE PANTETHINE FREAK B5
http://www.coenzyme-a.com/testimonial.html
Dear Coenzyme-A Technologies,
I’m 21 years old and I spent last year down in South America experiencing a very stressful and different lifestyle. I’ve always been a very healthy person with a great complexion. But I came back from South America a “different person”, suffering from acne that covered my entire face. I also came back due to a horrible internal discomfort that I thought might have been from parasites. So, for the last 4 months I’ve seen nearly every kind of doctor in Washington; I’ve seen Naturopaths, visited Tacoma General Hospital for a Western Medicine practitioners diagnosis, I’ve been put on Accutane, and its been like a guessing game for them all. Meanwhile as I took their herbs, pills, and medication, my constipation got so bad I’d have to count the days in waiting, and my depression was dragging me under to the point where I didn’t want to get up at all. The Accutane devoured my skin for a while and I felt like I had no face until I put the Accutane pills away and started taking Coenzyme-A Clear Skin Image instead.
I started taking 3 pills 3 times a day, 6 weeks ago. Almost immediately after I started, my bowel movements became regular. This was fantastic! I was still pretty depressed, but at least my system was being cleansed. Within the first 3 weeks my skin started shining and smoothing out and I stopped seeing a doctor.
My life has been smoothing out, and I know I’m on the right path at last. But just to test these beneficial resu1ts, I stopped taking the Clear Skin Image pills for a week. Things started slipping fast, I felt a little constipated and the internal discomfort started up again and I felt more depressed. Before damage could be done to my face I got another bottle of Clear Skin Image. I want to be on the Coenzyme-A Clear Skin Image pills for a longer period of time. This product has proven itself to be the total mind/body remedy we’ve all been looking for. I hope others have the good fortune to find this product too. Thank you guys so much, I can’t even express the relief and gratitude I feel now. I love the continuous results.
Mucous Gracias, Jesse A. Morrison Seattle, Washington
Lupus
http://www.ncbi.nlm.nih.gov/pubmed/13985157
Vestn Dermatol Venerol. 1963 Mar;37:16-20. [Combined treatment of lupus erythematosus patients with resochin and calcium pantothenate.][Article in Russian] TISHCHENKO LD.
http://www.ncbi.nlm.nih.gov/pubmed/13423891
AMA Arch Derm. 1957 Jun;75(6):845-50.The diagnosis of lupus erythematosus; probable significance of pantothenate blood levels.SLEPYAN AH, FROST DV, OVERBY LR, FREDRICKSON RL, OSTERBERG AE.
43. Cochrane, T., Leslie, G. (1952). The treatment of lupus erythematosus with calcium pantothenate and panthenol. J. Invest. Dermat., 18, 365-367.
http://www.journals.elsevierhealth.com/periodicals/ymehy/article/PIIS0306987704000945/abstract
Volume 62, Issue 6, Pages 922-924 (June 2004)
Systemic lupus erythematosus: a combined deficiency disease
Lit-Hung Leung1Received 12 July 2003; accepted 23 January 2004.
To date, the pathogenesis of systemic lupus erythematosus (SLE) remains unclear. By critically analyzing clinical facts and laboratory data, a hypothesis is proposed: drug-induced lupus erythematosus (DILE) is linked to a deficiency in Coenzyme A (CoA) that is secondary to a deficiency in pantothenic acid. This hypothesis is used to explain the high incidence of SLE in females, the role of sex hormones in this disease and the mechanism underlying a flare. The actions of anti-malarials and steroids are also discussed. The protean clinical presentation of SLE is attributed to co-existing deficiencies of dietary factors in addition to pantothenic acid. Contributing factors to these deficiencies may include increased nutritional requirements resulting from gene mutations. Treatment is replacement therapy with doses of pantothenic acid that is hundreds of times higher than that of the Dietary Reference Intake (DRI) and other vitamins. Using this method, 12 SLE females were studied with promising results.
http://www.mitamins.com/library/Concern/Lupus.html
51. Welsh AL. Lupus erythematosus: Treatment by combined use of massive amounts of pantothenic acid and vitamin E. Arch Dermatol Syphilol 1954;70:181–98.
46. Welsh (1952, 1954) reported an open study in which patients were treated with
extremely high doses of pantothenic acid derivatives, with the aim to alleviate
symptoms of lupus erythematosus. A total of 67 patients was treated, for periods of up
to 3 years, with daily doses* of calcium pantothenate (10-15 g), pantothenyl alcohol
(panthenol) (10-15 g) or sodium pantothenate (5-10 g), in combination with 1-2
mg vitamin E.
Some patients showed improvement of symptoms which the authors
considered to be related to the supplementation, although it was also noted that 11 patients developed new lesions whilst undergoing therapy. Symptoms of transient nausea and gastric distress were reported as the only side effects of the therapy. The authors also stated that “varying combinations and massive dosages of pantothenic acid derivatives and vitamin E preparations were given to 154 patients who had diseases other than lupus
http://archive.food.gov.uk/committees/evm/papers/evm0101.pdf
Cochrane T, Leslie G. The treatment of lupus erythematosus with calcium pantothenate and panthenol. J Invest Dermatol 1952;18:365–7.
An open study regarding the potential therapeutic effects of pantothenate supplementation in patients with lupus erythematosus was reported by Cochrane & Leslie (1952). A total of 37 patients was treated with daily doses of 600 mg calcium pantothenate (in the majority of cases the dose was 400 mg/day) for periods of 24 weeks. Improvement of disease symptoms was not observed in any of the treated subjects, although some cases worsened during the study period. No side effects of the therapy
Fair Use Notice:
The material on this site is provided for educational and informational purposes. It may contain copyrighted material the use of which has not always been specifically authorized by the copyright owner. It is being made available in an effort to advance the understanding of scientific, environmental, economic, social justice and human rights issues etc. It is believed that this constitutes a ‘fair use’ of any such copyrighted material as provided for in section 107 of the US Copyright Law. In accordance with Title 17 U.S.C. Section 107, the material on this site is distributed without profit to those who have an interest in using the included information for research and educational purposes. The information on this site does not constitute legal, medical or technical advice.
Disclaimer click here: http://www.drdach.com/wst_page20.html
The reader is advised to discuss the comments on these pages with his/her personal physicians and to only act upon the advice of his/her personal physician Also note that concerning an answer which appears as an electronically posted question, I am NOT creating a physician — patient relationship. Although identities will remain confidential as much as possible, as I can not control the media, I can not take responsibility for any breaches of confidentiality that may occur.
Link to this article: http://wp.me/P3gFbV-n2
(c) 2008-2013 Jeffrey Dach MD All Rights Reserved This article may be reproduced on the internet without permission, provided there is a link to this page and proper credit is given.
chelsea williams February 16, 2014 at 5:19 PM
My 14 year old son, has been taking 950 mg of Pantethine twice daily and 500 mg of L-Carnitine daily, for the last 4 weeks and 2 days. There is a SIGNIFICANT improvement in his complexion. He had cystic acne…those are gone! And then he had moderate acne bumps on his cheeks, one large bump on his nose and 2 large acne areas on his jawline. The bump on his nose is gone. The areas on his jawline are greatly diminished, and the areas on his cheeks are smoother and the bumps are not raised, and are less red. My husband had made an appointment with a dermatologist for later this month….and he is going to cancel the appointment tomorrow. I know 4 weeks seems like a long time…but compared to this going on for 2 years and we have tried EVERY over the counter cream, ointment, natural remedy, etc. Thank God my husband kept researching and found Dr. Dach’s article and Dr. Leung’s research! Amazing! It all makes sense, about the Co-enzyme A, and we feel that this is a cure…and it’s safe. Why would doctors put kids/teens on Accutane?!?! The side effects are so severe and dangerous. I wish everyone the best, and I hope the Pantethine works for you, too! By the way we buy ours from The Vitamin Shoppe.
Jeffrey Dach MD February 16, 2014 at 7:44 PM
Thanks for the follow up on the B5 for acne.